Second Child Birth Story
Youngest children may be spoiled, but in some ways they do get the short end of the stick. For example, my youngest child (known as J for this story) will be 2 years old this March, and I'm just now getting around to putting his birth story on "paper". The interesting thing is, it's the most amazing and miraculous birth story so far (of my two children).
The first part of the "miracle" is actually difficult to explain. I consider it a part of J's birth story, despite the fact that it was prior to his conception. We actually found out in January 2012 that we were expecting and started seeing a nurse-midwife since I was unhappy with my treatment at the multi-doctor practice I saw for our first child. Our first appointment at this new practice was supposed to be for our 12-week appointment and took place in March of 2012. Unfortunately, there was no heartbeat. An ultrasound eventually showed that a missed miscarriage happened. Sometime around the 5th or 6th week of pregnancy I had miscarried, but my body hadn't realized it. I did complete the miscarriage at home that week and only had to see an empty amniotic sac rather than a partially formed baby. I avoided the dreaded D & C, but did have to return several times to a very unsympathetic nurse for blood draws to make sure my hormone levels dropped appropriately.
You may think this is the opposite of a miracle, but I'll explain my reasoning at the end of the story.
Fast forward two full cycles after my hormones were regulated (the minimum amount the midwife told us to wait before getting pregnant again) and we were able to get pregnant again right away. Now, instead of our first and second children being two years apart, they would be almost exactly two and half years apart, with an expected due date of February 20th. Now, with the bad experience at the nurse-midwife and the person in charge of blood draw (I do not do well with needles and she would not allow my husband to come back with me during blood draws), I decided to choose yet another practitioner. This doctor attends the births for all her own patients, despite having an "On call" doctor and a multi-doctor practice, and delivers at the hospital with the best/highest level NICU in our area.
Based on an early ultrasound (due to the previous missed miscarriage), my due date was adjusted from February 20th to 26th. It was a relatively normal pregnancy. I didn't have the smell/taste aversions quite as bad as I did with D (firstborn). I also gained a lot of weight (about 60 pounds or so) which was about the same amount I gained in my first pregnancy. This time around, however, I carried all the weight in my belly. I never measured "large for dates" although I was asked in December if I was having a "Christmas baby" even though I was only 6.5 months pregnant, as well as if I was having twins.
Well, February 20th came and went with nothing more than a few bouts of Braxton Hicks contractions. I was disappointed, but thought that I would certainly give birth by my adjusted due date of February 26th. On February 25th my doctor said that she would "talk about inducing" at the next appointment, but not to worry about it yet. Finally, on February 28th, I went into labor. I knew it was the real thing, because I had experienced the real thing before. It was very similar to my early labor with my first born, except for one major difference, I had unfortunately caught the stomach bug the same day I went into labor.
Very similar to my first labor, I was originally told by the hospital to go home and rest. I tried, but this time around "resting" was laying on my side on our bed and then getting up every hour to sit on the toilet with a trash can in front of me. I could not hold down any liquid or even ice chips, so I finally checked myself back into the hospital and told them they had better keep me this time and that I needed an IV (again I hate needles, so this was desperation). I knew I needed something to help me get through labor. I will say that a sugar IV was the best thing that ever happened to me at this point, I desperately needed some energy and hydration.
Fortunately, the third time they gave me anti-nausea medicine, it seemed to work, and I was able to rest for a little while as my labor progressed. I still refused an epidural, and my angel of a doctor had no problem with that. However, as I got into the transition stage, it was really hard to get over the mental hurdle from being sick all day. The pain was just overwhelming and I was not able to handle it as well as with my first born. I did eventually ask for and receive some pain medicine through the IV, which allowed me to rest between contractions.
Finally, just after midnight on March 1st, I started to push. After about a half hour of pushing, the doctor started to act a little worried. There was a lot of meconium in the fluid. After a few more pushes she was able to see the baby's head. She asked for a nurse to bring in her "instrument bag". It sounded like she thought he was breech, but I wasn't concerned about that because I could tell that he was head down. After a little over an hour of pushing, and after alerting the NICU unit because of the meconium, she said that we would need to use vacuum suction to help him out a little more quickly. At that point, I was up for anything that would get him out more quickly.
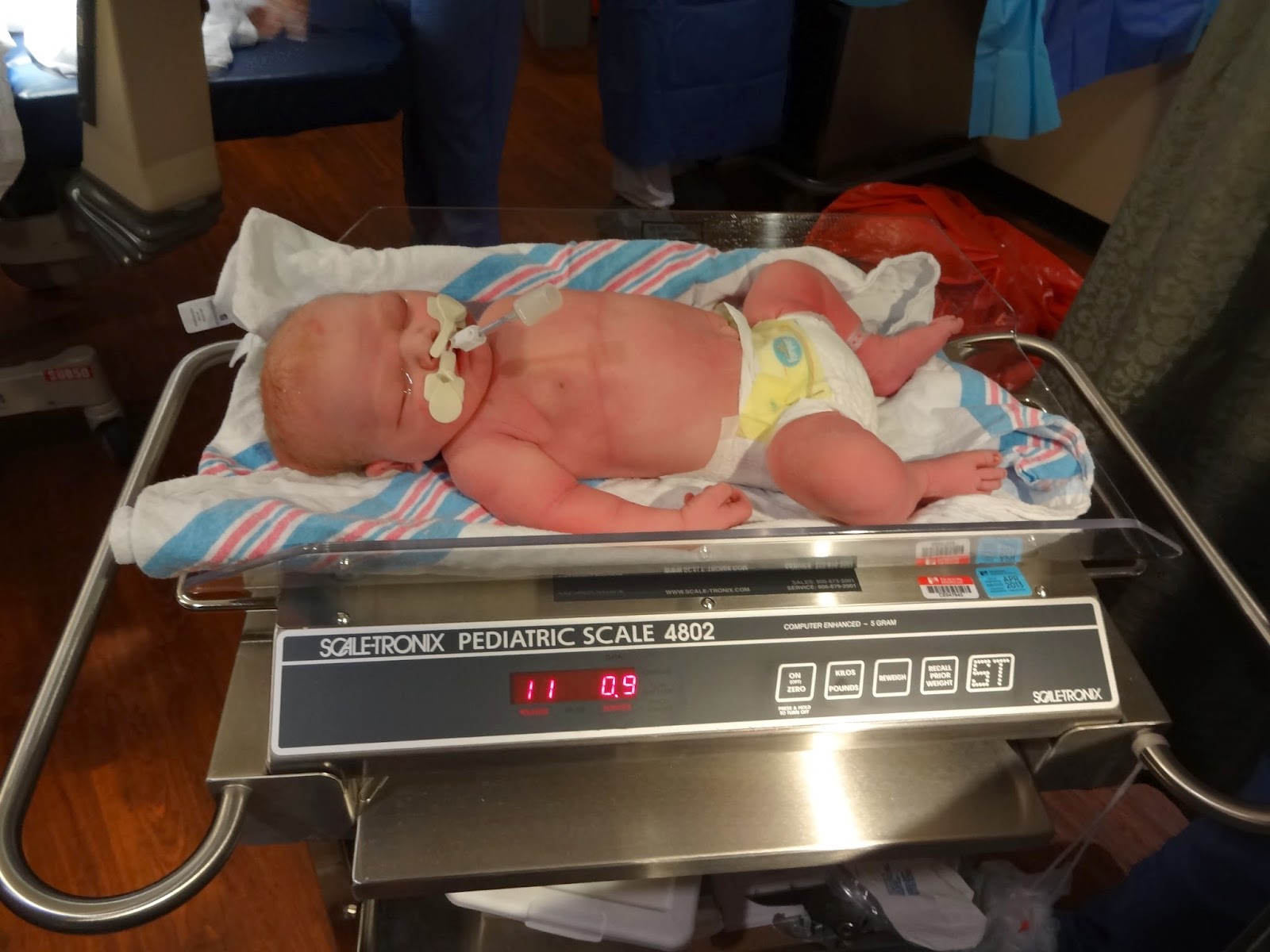
After one or two successful attempts with the vacuum assistance, his head finally came out, followed quickly by his shoulders and body. The NICU team quickly took over and had the baby intubated, cleaned, and diapered before the doctor finished delivering the placenta. We were able to hold him for a few minutes before the NICU team whisked him off to be treated for meconium aspiration. He had a very low 1-minute Apgar score (I believe it was either 3 or 5) but since he was being treated right away, no one seemed terribly concerned. After being intubated he perked up quite nicely, and seemed like a perfectly normal healthy baby, despite being a bit big. He weighed 11 pounds 1 ounce after being intubated and having a newborn diaper on. He was 22 inches long.
My husband went with the baby to the NICU and I was transferred to a recovery room. After my husband came back down from the NICU, he ran home to change out babysitters for our older son and grab some food. While he was still gone, one of the NICU doctors and the "on-call" doctor from my doctor's practice came to my hospital room. It's never encouraging when there are two doctors coming to talk to you. They said that J was having seizures due to hypoxic ischemia and needed to be treated right away. They had actually already started the treatment by giving him anti-seizure medicine (it took 3 medicines to find one that worked), but they wanted to let me know what was happening. The other treatment they wanted to try was brand-new. Sometime in January of that year, this hospital had received their first "cooling blanket" to treat infants with hypoxia. They would cool down his body to create a hypothermic state and he would stay in that state for 3 days. It was the only treatment available that had a chance of working, so I agreed to start that treatment and called my husband right away to let him know. Essentially, the anti-seizure medicines could stop the seizures, but there was still what they called "suppression activity" on the EEG which meant that the brain damage was worsening.
The first time I saw my son in the NICU his toes were already blue and he was sedated so he wouldn't pull off the many wires and tubes. However, I was also told that only a short time after being put on the cooling blanket, the EEG showed that the suppression activity stopped and the brain waves were completely normal. After 8 total days in the NICU the top pediatric neurologist in the state said that he was cautiously optimistic that J would make a full and complete recovery with no brain damage.
I know it was a miracle that this was the only hospital in the area with that specialized equipment. The equipment had only arrived a few months before my son was born and needed it. He was already in the NICU for meconium so the doctors and nurses recognized the seizure signs right away and got him treatment right away. If I hadn't had a miscarriage and the same scenario happened, he would not have had access to this treatment. When I first heard the diagnosis, I wondered how much brain damage there would be, now I only wonder how I will keep up with my smarty-pants 20 month old who has a 200+ word vocabulary and chases/climbs/jumps to keep up with his big brother. He is above average on all the developmental tests, and his neurologist has completely cleared him.
Every time I visit the pediatrician, she marvels at this "perfect" child and tells everyone what his original diagnosis was. I think I never realized exactly how bad the situation could have been until we were required to speak with a social worker prior to J's discharge because of his diagnosis. She was so serious discussing all of the treatments available and I was just so excited that the neurologist thought he would be fine. I know many parents are dealing with treatment plans and therapies and we did have a few extra follow up appointments in the beginning. I pray every time I see one of my friends who are dealing with speech therapy or epilepsy or babies who have died at 3 or 10 months old from various conditions. I know that bad things do happen to good people and we don't always understand why. Maybe we won't understand until we get to heaven, or maybe the answer is that evil and death and suffering exist in this world. I also know, that in this case, one bad thing did happen, but a miracle happened too, and I'm so excited to see the plans God has for my spoiled rotten almost-two year old.
The first part of the "miracle" is actually difficult to explain. I consider it a part of J's birth story, despite the fact that it was prior to his conception. We actually found out in January 2012 that we were expecting and started seeing a nurse-midwife since I was unhappy with my treatment at the multi-doctor practice I saw for our first child. Our first appointment at this new practice was supposed to be for our 12-week appointment and took place in March of 2012. Unfortunately, there was no heartbeat. An ultrasound eventually showed that a missed miscarriage happened. Sometime around the 5th or 6th week of pregnancy I had miscarried, but my body hadn't realized it. I did complete the miscarriage at home that week and only had to see an empty amniotic sac rather than a partially formed baby. I avoided the dreaded D & C, but did have to return several times to a very unsympathetic nurse for blood draws to make sure my hormone levels dropped appropriately.
You may think this is the opposite of a miracle, but I'll explain my reasoning at the end of the story.
Fast forward two full cycles after my hormones were regulated (the minimum amount the midwife told us to wait before getting pregnant again) and we were able to get pregnant again right away. Now, instead of our first and second children being two years apart, they would be almost exactly two and half years apart, with an expected due date of February 20th. Now, with the bad experience at the nurse-midwife and the person in charge of blood draw (I do not do well with needles and she would not allow my husband to come back with me during blood draws), I decided to choose yet another practitioner. This doctor attends the births for all her own patients, despite having an "On call" doctor and a multi-doctor practice, and delivers at the hospital with the best/highest level NICU in our area.
Based on an early ultrasound (due to the previous missed miscarriage), my due date was adjusted from February 20th to 26th. It was a relatively normal pregnancy. I didn't have the smell/taste aversions quite as bad as I did with D (firstborn). I also gained a lot of weight (about 60 pounds or so) which was about the same amount I gained in my first pregnancy. This time around, however, I carried all the weight in my belly. I never measured "large for dates" although I was asked in December if I was having a "Christmas baby" even though I was only 6.5 months pregnant, as well as if I was having twins.
Well, February 20th came and went with nothing more than a few bouts of Braxton Hicks contractions. I was disappointed, but thought that I would certainly give birth by my adjusted due date of February 26th. On February 25th my doctor said that she would "talk about inducing" at the next appointment, but not to worry about it yet. Finally, on February 28th, I went into labor. I knew it was the real thing, because I had experienced the real thing before. It was very similar to my early labor with my first born, except for one major difference, I had unfortunately caught the stomach bug the same day I went into labor.
Very similar to my first labor, I was originally told by the hospital to go home and rest. I tried, but this time around "resting" was laying on my side on our bed and then getting up every hour to sit on the toilet with a trash can in front of me. I could not hold down any liquid or even ice chips, so I finally checked myself back into the hospital and told them they had better keep me this time and that I needed an IV (again I hate needles, so this was desperation). I knew I needed something to help me get through labor. I will say that a sugar IV was the best thing that ever happened to me at this point, I desperately needed some energy and hydration.
Fortunately, the third time they gave me anti-nausea medicine, it seemed to work, and I was able to rest for a little while as my labor progressed. I still refused an epidural, and my angel of a doctor had no problem with that. However, as I got into the transition stage, it was really hard to get over the mental hurdle from being sick all day. The pain was just overwhelming and I was not able to handle it as well as with my first born. I did eventually ask for and receive some pain medicine through the IV, which allowed me to rest between contractions.
Finally, just after midnight on March 1st, I started to push. After about a half hour of pushing, the doctor started to act a little worried. There was a lot of meconium in the fluid. After a few more pushes she was able to see the baby's head. She asked for a nurse to bring in her "instrument bag". It sounded like she thought he was breech, but I wasn't concerned about that because I could tell that he was head down. After a little over an hour of pushing, and after alerting the NICU unit because of the meconium, she said that we would need to use vacuum suction to help him out a little more quickly. At that point, I was up for anything that would get him out more quickly.
After one or two successful attempts with the vacuum assistance, his head finally came out, followed quickly by his shoulders and body. The NICU team quickly took over and had the baby intubated, cleaned, and diapered before the doctor finished delivering the placenta. We were able to hold him for a few minutes before the NICU team whisked him off to be treated for meconium aspiration. He had a very low 1-minute Apgar score (I believe it was either 3 or 5) but since he was being treated right away, no one seemed terribly concerned. After being intubated he perked up quite nicely, and seemed like a perfectly normal healthy baby, despite being a bit big. He weighed 11 pounds 1 ounce after being intubated and having a newborn diaper on. He was 22 inches long.
My husband went with the baby to the NICU and I was transferred to a recovery room. After my husband came back down from the NICU, he ran home to change out babysitters for our older son and grab some food. While he was still gone, one of the NICU doctors and the "on-call" doctor from my doctor's practice came to my hospital room. It's never encouraging when there are two doctors coming to talk to you. They said that J was having seizures due to hypoxic ischemia and needed to be treated right away. They had actually already started the treatment by giving him anti-seizure medicine (it took 3 medicines to find one that worked), but they wanted to let me know what was happening. The other treatment they wanted to try was brand-new. Sometime in January of that year, this hospital had received their first "cooling blanket" to treat infants with hypoxia. They would cool down his body to create a hypothermic state and he would stay in that state for 3 days. It was the only treatment available that had a chance of working, so I agreed to start that treatment and called my husband right away to let him know. Essentially, the anti-seizure medicines could stop the seizures, but there was still what they called "suppression activity" on the EEG which meant that the brain damage was worsening.
The first time I saw my son in the NICU his toes were already blue and he was sedated so he wouldn't pull off the many wires and tubes. However, I was also told that only a short time after being put on the cooling blanket, the EEG showed that the suppression activity stopped and the brain waves were completely normal. After 8 total days in the NICU the top pediatric neurologist in the state said that he was cautiously optimistic that J would make a full and complete recovery with no brain damage.
I know it was a miracle that this was the only hospital in the area with that specialized equipment. The equipment had only arrived a few months before my son was born and needed it. He was already in the NICU for meconium so the doctors and nurses recognized the seizure signs right away and got him treatment right away. If I hadn't had a miscarriage and the same scenario happened, he would not have had access to this treatment. When I first heard the diagnosis, I wondered how much brain damage there would be, now I only wonder how I will keep up with my smarty-pants 20 month old who has a 200+ word vocabulary and chases/climbs/jumps to keep up with his big brother. He is above average on all the developmental tests, and his neurologist has completely cleared him.
Every time I visit the pediatrician, she marvels at this "perfect" child and tells everyone what his original diagnosis was. I think I never realized exactly how bad the situation could have been until we were required to speak with a social worker prior to J's discharge because of his diagnosis. She was so serious discussing all of the treatments available and I was just so excited that the neurologist thought he would be fine. I know many parents are dealing with treatment plans and therapies and we did have a few extra follow up appointments in the beginning. I pray every time I see one of my friends who are dealing with speech therapy or epilepsy or babies who have died at 3 or 10 months old from various conditions. I know that bad things do happen to good people and we don't always understand why. Maybe we won't understand until we get to heaven, or maybe the answer is that evil and death and suffering exist in this world. I also know, that in this case, one bad thing did happen, but a miracle happened too, and I'm so excited to see the plans God has for my spoiled rotten almost-two year old.

Comments